July 10, 2017
The pharmaceutical industry is rapidly changing with the growing popularity of biologics and biosimilars. In fact, more than 60 percent of patent filings are made on behalf of the industry’s top-ten biologics companies.1 Due to the effectiveness of biologics and biosimilars in treating and managing chronic conditions, biopharmaceuticals are seeing an annual growth rate of more than 8 percent, comprising 20 percent of the pharma market. 2
Concurrently, the combination product market is continuing to grow with autoinjectors remaining a preferred drug-delivery device for chronic disease management. More than 50 biologic medications and vaccines are currently delivered in prefilled syringes, including prefilled syringes enclosed in autoinjectors, and more than 3.5 billion prefilled syringe units are produced to be used by patients and healthcare providers around the globe each year. 3,4
While biopharmaceuticals have been found to be extremely effective and autoinjectors are believed to offer an improved patient experience compared with other injection systems, administration errors and device misuse can lead to lower adherence, injuries, and suboptimal treatment outcomes. With the self-administration challenges patients continue to face, pharmaceutical teams offering comprehensive, patient-centric training and onboarding platforms to decrease errors and counteract other factors could decrease the cost of nonadherence to the brand and ultimately the healthcare system.
Causes of Nonadherence
A study conducted by the University of Texas Medical Branch at Galveston (UTMB) found that 84 percent of patients failed to properly use an autoinjector, with more than 50 percent missing up to four steps. The study also found that “wet injections,” which result in patients not receiving the full prescribed medication dosage, were the most common type of patient error, comprising 76 percent of errors made. 5 There are several contributing factors that can result in improper administration technique and nonadherence.
Even before a healthcare professional delivers a diagnosis and training to a patient, there could be confusion. Healthcare professionals receive training on proper administration techniques for multiple drug-delivery devices that could include a variety of different device administration techniques. Training with multiple devices could result in confusion when correctly recalling the operational sequence and functionality for a particular device or when relaying this information to patients. On the patient’s end, findings suggest that 40-80 percent of medical information provided by healthcare providers is forgotten immediately possibly due to shock, sadness, confusion, or other cognitive and emotional factors. 6, 7
After diagnosis, the first 30-, 60-, 90-days, and beyond (a time also known as “onboarding”) are the most important times for patients regarding adherence with several factors impacting the onboarding process. Training decay, lack of comprehensive training materials, and anxiety are just a few causes of nonadherence. To counteract these factors, patients need patient-centric educational resources during onboarding to reduce training decay, decrease anxiety, and build patient confidence. One drug-delivery component that offers an additional touch point for training is drug-delivery device packaging. By reinforcing training via packaging, pharmaceutical teams can help patients in the following five key ways.
How Packaging Can Help
1. Reducing Anxiety
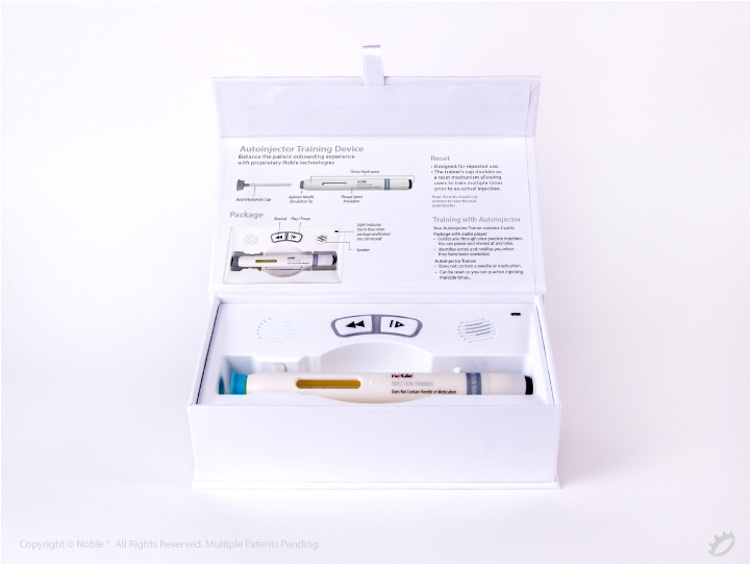
Studies have shown that 45 percent of patients skip or avoid injections during the onboarding timeframe due to anxiety or fear. 8 One key factor that can help reduce anxiety is providing training prior to and after the first injection. This training builds confidence and reduces anxiety, which decreases the risk that the patient will engage in avoidance behaviors. For example, Noble’s Smart Packaging training platform, which leverages a drug-delivery device trainer and smart packaging with error-correcting audible feedback to walk patients through administration steps, allows patients to repeatedly practice self-injection technique at home.
2. Increasing Memory Recall
Packaging allows for various platform technologies that can provide multisensory feedback. Designs could include visuals, audio, LEDs that correspond to auditory script, and more. Studies have shown that stimulating multiple areas of the brain during training improves recall and retention of educational messaging. These features not only improve memory recall between dosages, but also help to reduce the learning curve as patients are using multiple senses to reinforce training through learning and experience. 9
3. Providing Interactive Feedback
Interactive feedback is another packaging feature that can help reinforce message and training recall. Noble’s Smart Package training platform also includes sensors that are digitally connected to the device packaging to alert the patient when mistakes are made. Further, the technology does not enable patients to move forward in the administration process until the step is corrected. This builds muscle memory and diminishes the likelihood that patients will develop non-adherent behaviors, such as skipping steps in the administration process.
4. Using Technology to Shorten the Learning Curve for Specific Errors
By including technology in packaging as part of the training and onboarding process, companies are able to focus training on specific critical errors related to a device. Although all self-administration steps are covered, the ability to highlight a specific sequence of the administration process and reinforce correct technique can help reduce the most detrimental of administration errors. For instance, wet injections were one of the most common patient errors for autoinjectors. Error-correcting technologies in packaging could include messaging with more emphasis on tactile and audible feedback, plunger speeds, and dose completion signals to help patients establish administration timeframes and reduce the likelihood of a wet injection ensuring the patient receives the full dose.
5. Preventing Training Decay
Training decay can result from time-lapsed, diminished memory recall of technique and incorrect recollection of the treatment dosing schedule. To counteract training decay, patients need a reminder that goes beyond Instructions for Use (IFU) when explaining the drug-delivery device’s operational sequence. A recent study conducted by Noble found that nearly two-thirds of patients don’t thoroughly read IFU documents prior to treatment. Incorporating training aids that offer additional educational support into packaging gives patients the opportunity to relearn or reinforce training in an engaging manner throughout the course of treatment.
Packaging should be considered an essential part of the training process. As biopharmaceuticals and corresponding drug-delivery devices like the autoinjector continue to grow in popularity, so too will the need to improve the patient onboarding experience with comprehensive training. As more biologic medications are being developed, brands will need to differentiate themselves as they launch their medications into this competitive environment. A well-informed and trained patient not only results in improved treatment outcomes, but also drives brand preference for the healthcare provider. Providing an optimal onboarding experience may be the factor that brands need to gain essential competitive edge.
Paul Sullivan serves as associate director, business development at Noble.
References
Don't miss the MD&M Minneapolis Conference and Expo, November 8–9, 2017.
About the Author(s)
You May Also Like


